Softwave: for Faster Healing & Pain-Free Living
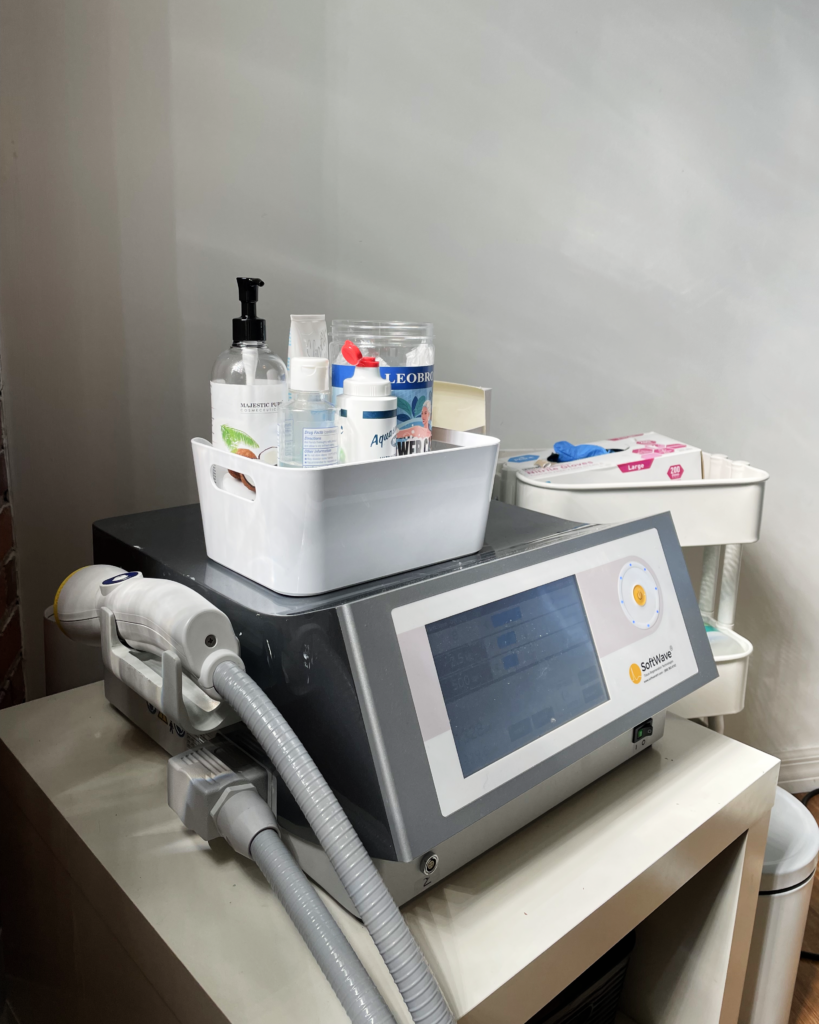
Softwave Therapy is a unique form of treatment that uses shockwaves to encourage the body’s natural healing response. This form of therapy has been researched and developed since the 1950s. The treatment itself is fast, pain-free, and brings results quickly! Softwave TRT is the machine we use at BPHAC, and it is the top-of-the-line technology when it comes to Shockwaves and ESWT.
“SoftWave is currently the only company that offers broad focused true shock wave technology in their devices. The therapy provided by a SoftWaveTRT device has a wider and deeper therapeutic energy zone than other ESWT devices on the market. This results in greater healing as the energy is spread over a vastly larger and deeper area.” –https://softwavetrt.com/faq/
How does it work on a scientific level?
The applicator device generates a large positive pressure wave followed by a negative pressure wave. The tissues in your body react to this stimulus with a biochemical reaction, and sends signals to your cells. The resulting biological response is: Angiogenesis (formation of new blood vessels), inflammatory modulation, stimulation of tissue regeneration.
In more direct words; sending shockwaves into soft-tissue that is injured, scarred, contains adhesions, or is painful/inflamed helps the body jumpstart its own natural healing process, on the cellular level. More blood flow and less inflammation lead to less pain!
This specific machine is impressive because the specialized applicator offers a true shockwave – not all machines or similar therapies on the market do this. It also has a wider and deeper range for affecting the tissue, increasing your healing. You can dive into the nitty gritty science of it at Softwave’s website here! https://softwavetrt.com/softwave-technology/
What can it treat?
Lots of things! We use Softwave in the clinic daily to treat shoulder and back pain, foot/knee pain, arthritis and bursitis, chronic pelvic pain and erectile dysfunction, and more. A more complete list can be found at our website here
If you really want a deep dive, the published research on Softwave is extensive and exciting! See below- we love perusing this page in our down time 🙂
Some of our favorite in-clinic Softwave Win moments…
“Great provider. Very knowledgeable. Add some shocks to other problem spots. Feeling good. Shockwave therapy is good for a wide variety of ailments.” -Keith
“Got me out of intense pain within 24 hours! Softwave with Nicole was quick and pain-free- not sensationless, but not painful. I was experiencing neck pain and headaches that would not give up, no matter what I tried. A session of Softwave and one full day later, I feel 100% better. Nicole walked me through her process every bit of the way and made sure I was comfortable and knew what to expect for the whole treatment.” -Lindsey
“Can I give 6 stars??!” -Dave
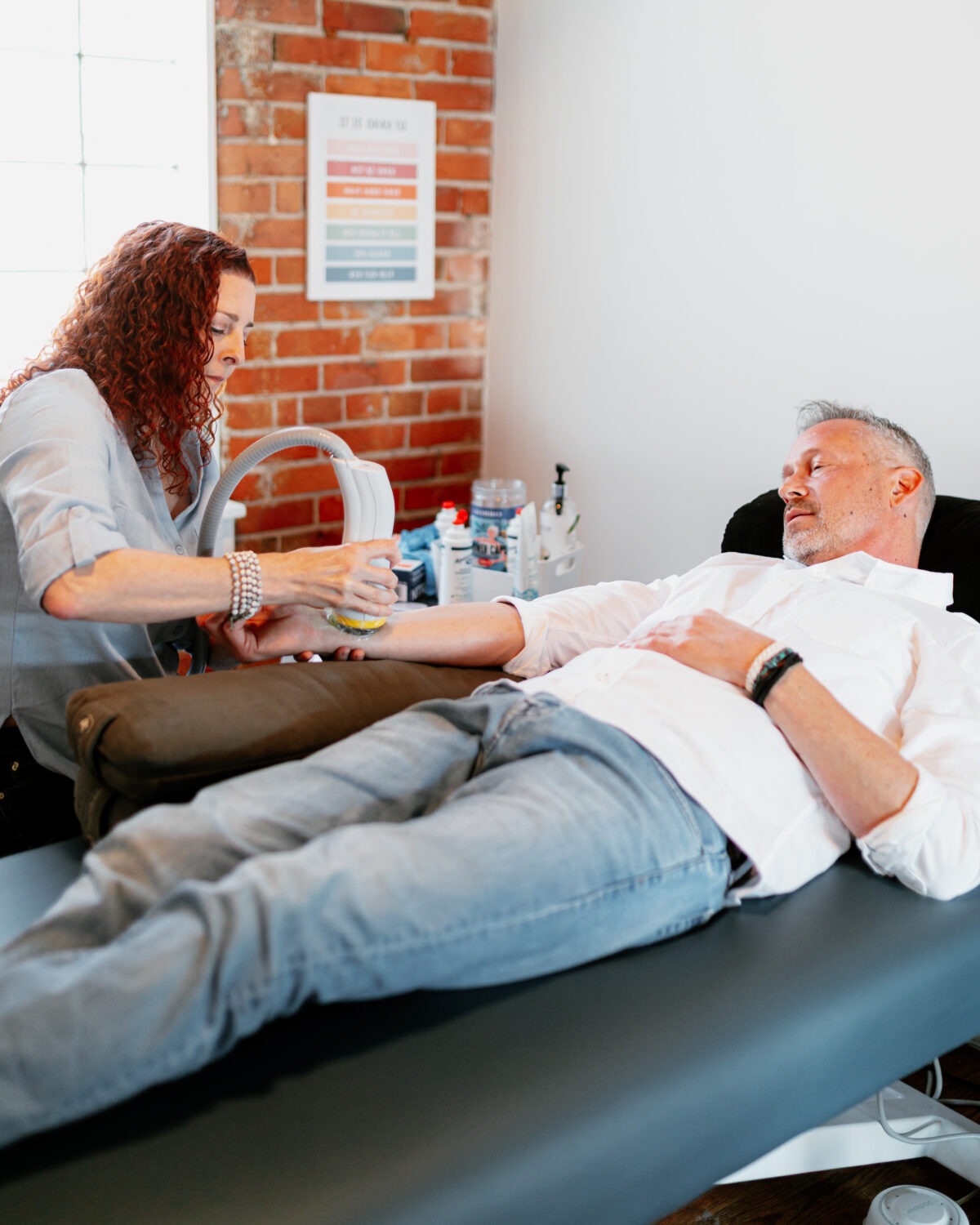
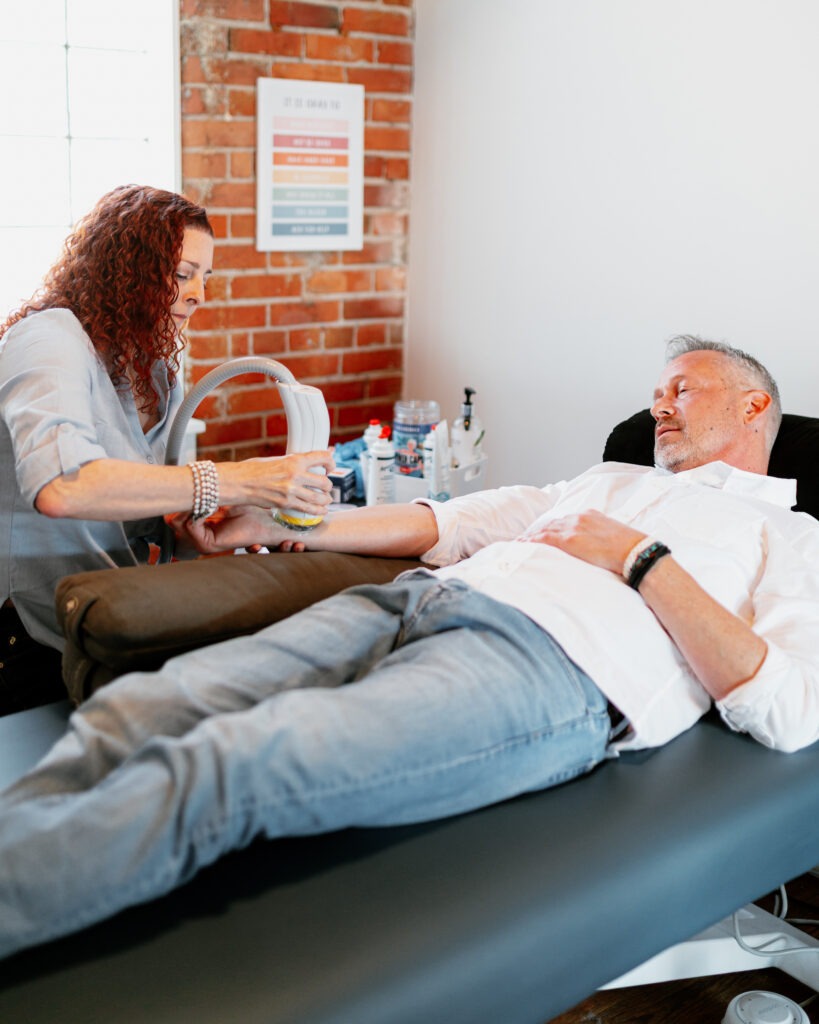
What an average session looks like:
Softwave sessions at BPHAC are quick and easy! If you’re running on a busy schedule, this is an ideal way to address pain in a shorter time frame. Coming in for a follow up, you’ll spend the first few minutes chatting with your practitioner about how you’ve been feeling recently since your last session. Be sure to notify them of all that you’ve noticed, good and bad!
If we’re focusing on pelvic health, or an area of the body that requires an outfit-change, the practitioner will leave the room and give you a moment to undress and cover up with a freshly laundered sheet. If it’s a body part that is a little more accessible, like a wrist or a foot, we will probably dive right into treatment after checking in and reassessing.
An ultrasound gel is applied to the area being treated, and your practitioner will move the applicator around the treatment area as the machine produces the shockwave pulses. Your practitioner will be sure to ask you for updates as we move along the tissue- some areas feel a bit like “hot spots”, and we may adjust the intensity of the machine if it feels like too much, or stay on that spot a bit longer, comfort level depending. Either way, you and your practitioner will be in communication the whole time about the intensity level and how things are feeling. A usual Softwave Follow Up at BPHAC is 1500 “shocks” worth of treatment. Erectile Dysfunction treatment sessions are a pinch longer, administering 3000 shocks.
Combining Care
Due to the ease and effectiveness of Softwave Therapy, it is a great addition and supplement to other healing modalities. There is a good reason our acupuncturists and physical therapists here love it! Oftentimes pain can be the main barrier that prevents us from getting better. Pain is a symptom, not the root cause of dysfunction. Softwave treatments take away the barrier of pain, so our practitioners can fix the root problem. Oftentimes, patients leave a Softwave session feeling immediate pain relief.
If Softwave is something you’d like to add into your acupuncture or PT appointment, we do offer combo sessions, so you can get both treatments in one visit.
Most people walk away from the first session feeling the results. Generally, patients are seen weekly for 4-6 weeks to ensure best outcomes and lasting progress, then are put on a “maintenance” or “as-needed” follow up plan.
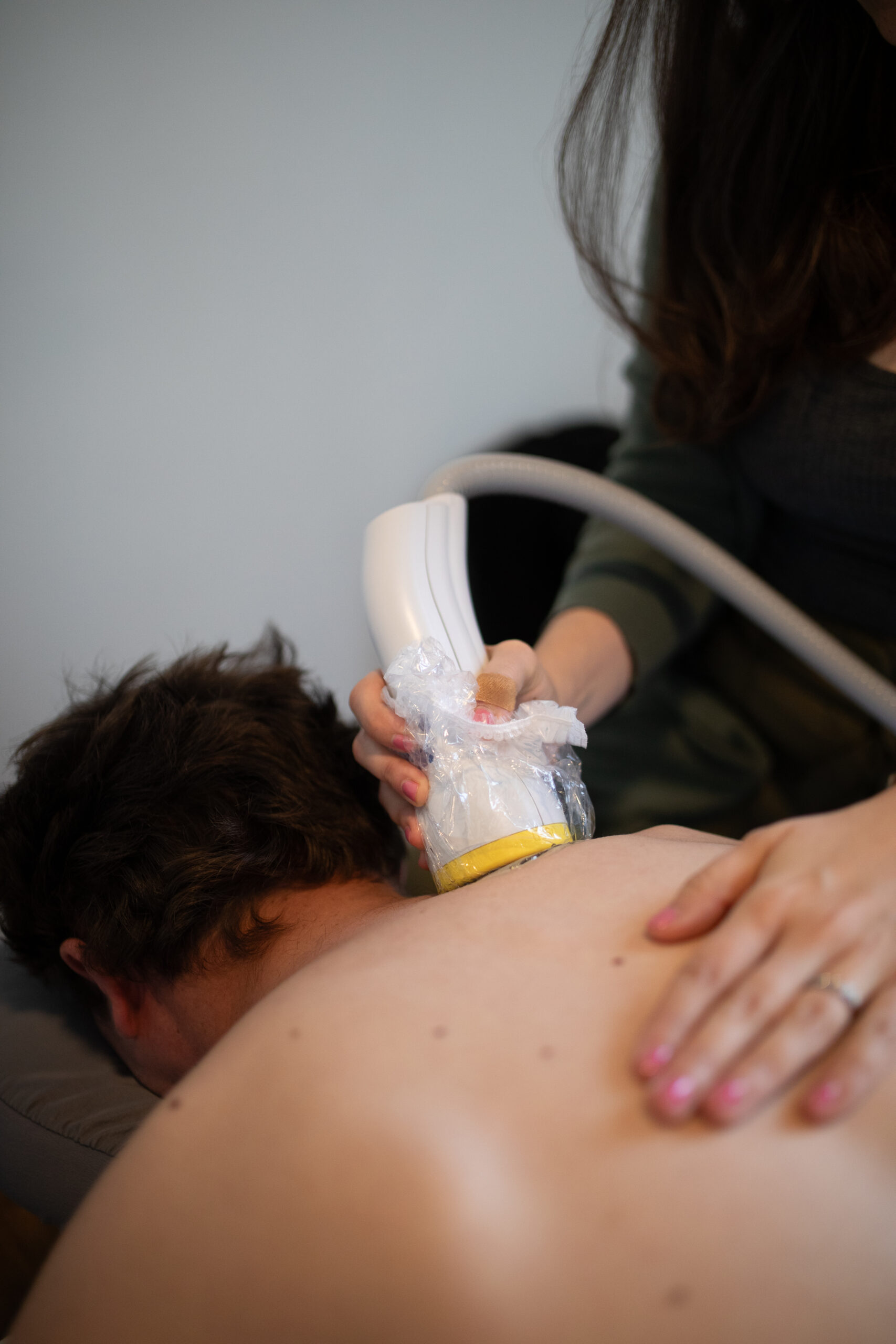
Doesn’t Shockwave hurt?
While not sensationless, Shockwave treatment should not be painful. Communicate to your practitioner if a certain level of intensity feels like too much for you- we can easily adjust the level of the machine, to ensure best results and a pain-free experience. Some mild discomfort or soreness shortly after treatment may occur, but most just experience a mild tapping or snapping sensation on the skin during treatment. https://softwavetrt.com/does-shockwave-therapy-hurt/
Getting the most out of your recovery:
Be sure to communicate to your practitioner what you are feeling during treatment. If you notice any changes in sensation, or if you’d like the intensity adjusted- this is all important information for your provider to ensure you get the best treatment.
While you can return right away to your daily routine after a softwave appointment, it is recommended to avoid high-impact activities for a day or two to the area after treatment.
And, as always, make sure you have your follow up booked according to your practitioner’s guidance! Much like acupuncture or physical therapy, waiting too long in between appointments can often hinder the progress previously made. These approaches are cumulative, and we aim to get you to that “maintenance” or “as-needed” phase of healing as soon as possible.